
MDA Ambassador Guest Blog: My Pompe Journey
By Kathryn Arvidson | Friday, April 10, 2026
5 Second Summary
MDA Ambassadors play an essential role in furthering MDA’s mission while representing and empowering the neuromuscular disease community. Quest Ambassador Guest Blog series provides a platform to share their personal stories, perspectives, and experience.
Kathryn Arvidson champions accessible mental health treatment for people with disabilities. Kathryn was diagnosed as a child with a rare degenerative neuromuscular disorder, Pompe disease, that impacts her mobility and pulmonary functioning. Kathryn earned a master’s degree in social work and served as a Licensed Clinical Social Worker and supervisor for licensed professional counselors in the fields of mental health, disabilities, and developmental disabilities. With her professional background in mental health treatment and her lived experience, Kathryn weaves a compelling story about thriving, resilience, and hope. As the previous Ms. Wheelchair Alaska USA, Kathryn, uses her platform “Moving Beyond Surviving, to Thriving” to create positive change for people living with a disability. Kathryn considers herself an advocate, changemaker, warrior, leader, truth teller, and optimist.

Kathryn Arvidson
My journey with Pompe disease began as a little girl. One evening, while washing dishes when I was 9 years old, I melted down. Crying in a way my mom had never heard before. A cry that was desperate. Something was wrong. My pediatrician ran bloodwork that revealed elevated liver enzymes, but no one could explain why. And so, my diagnostic journey began. Doctors, tests, and needles became routine. I wasn’t yet experiencing any symptoms that would help explain the elevated enzymes.
Finding answers
For the next three years, my life revolved around medical appointments and procedures. Often painful and frightening, these tests were necessary to rule out diagnoses. One particular test is burned into my memory: large needles placed deep into my muscles, an electrical current running between them, doctors telling me to contract the impacted muscles. They were measuring the health of my skeletal muscles and nerves. It was horrendous. That pain is unforgettable.
Eventually, a doctor performed a muscle biopsy, removing a small piece of my thigh to send for testing. A few months later, Dr. Greenburg, an endocrinologist, sat me down and delivered the news.
“Katy, you have a disorder called Pompe disease. You will not graduate from high school. You will not live to see adulthood. You have a muscle wasting disease. There is no treatment. You should not exercise or take part in athletics,” he said.
Not fully understanding the magnitude of what he was saying, my little-girl brain replied, “Well, I guess if I can’t be an athlete, I’ll be a Supreme Court judge.” In that moment, my life changed forever. I responded with resilience in the face of death, having no idea what the diagnosis would mean for my body or my future. There was nothing to do except continue living and moving forward.
Fighting for a future
At that time there was little to no information about Pompe disease. There was not a distinction made between Infantile Onset Pompe Disease (IOPD) and Late Onset Pompe Disease (LOPD). Babies with IOPD produce significantly less of the enzyme needed to break down glycogen in the body, causing damage to the heart muscle, and typically leading to death within the first year of life. People with LOPD may begin experiencing symptoms anytime between childhood into late adulthood and have a far wider range of symptom onset and severity.
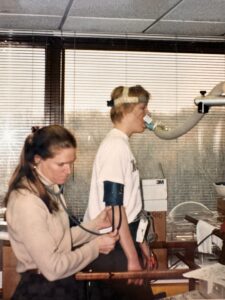
Kathryn Arvidson testing pulmonary functioning during the clinical trials.
Although I had this diagnosis hanging over my head, along with a strange sense of my own mortality, I ignored it as much as possible. I was a good student, loved theater, and wanted to attend college someday. I focused on all the normal teenage things: friends, school, and building a future for myself. I was determined to make a difference in the world. Even toward the end of high school, I wasn’t experiencing the symptoms I’d been told I would. It was easy to ignore. I did go on to college and graduate school. I decided I wanted to be a mental health therapist and work with children and families. My determination to put good into the world, took me down this path. It wasn’t until my junior year in college that I began experiencing symptoms. I started having a difficult time climbing stairs and had to begin using the elevator. I couldn’t carry my heavy backpack anymore. I would trip and fall if I wasn’t careful about how I was walking. In my mid-twenties, a clinical trial began for the first-ever Pompe treatment. Every two weeks, I traveled from Alaska to New York City, a trip that took twenty hours each direction. The clinical trial was double-blind, so I did not know whether I was getting the medication or a placebo. With hope and a prayer, I boarded an airplane every two weeks for three years, and then to Seattle for another two years. By this time, I relied on a cane to help me walk short distances and a collapsible scooter for longer distances. The grueling travel, combined with full-time work, shredded me physically and emotionally. I lived my life in a never-ending cycle of two-week increments: pack, fly, treatment, fly, unpack, work, repeat. We had to make tough decisions to keep me in the trial. Before every treatment, I would pee on a stick, confirming I was still childless. My marriage disintegrated. I drank alcohol to numb my grief. Even though the clinical trial was onerous, I honestly believe it saved my life. I did not know it at the time, but I had been receiving the enzyme replacement treatment, Myozyme, throughout the clinical trial. I do not think I would still be alive if I hadn’t started receiving the treatment when I did.
Two things sustained me through the clinical trial. The first was a quiet garden in Central Park where I’d eat my favorite deli sandwich and watch the seasons shift, grounding myself in time. I found peace, routine, and hope in my garden. The second was the excitement and joy of the young women who accompanied me each trip, most traveling to NYC for the first time. The pharmaceutical company allowed me to bring a companion each trip to help with luggage, my scooter, and travel. We would save our per diem and buy cheap tickets to see Broadway plays. Their joy and excitement gave meaning to the otherwise brutal schedule.
Despite the treatment, my body was failing. The Pompe disease continued to progress. Falls and concussions increased. I feared falling in the snow, unable to stand up independently. I made the decision to leave the work that filled my life with purpose. I had sacrificed nearly everything to stay in the clinical trial and now I had to walk away from my career. My drinking worsened. My grief was almost unbearable.
Moving beyond surviving

Kathryn Arvidson whale watching with her niece.
When I was in my early thirties, I received my first wheelchair. I fought to walk as long as I could, pain coursing through my body each step that I took. Even the bottoms of my feet hurt, desperately gripping the floor to prevent falls. First, I used the wheelchair only outside and for long distances and then, all the time. One day, I never stood again. By age 33 I was completely dependent on my wheelchair. What I did not understand at the time is that the wheelchair would give me more freedom and independence. It felt like I was giving up. Like I was quitting. But, I wasn’t. I was facing my life and making decisions to keep moving forward. To keep showing up.
I need help with almost everything now– getting out of bed, showering, dressing, driving. I’ve built a loving community around me that not only meets my physical needs, but helps me live out my dreams. My deep sense of service and putting something good into the world is again my focus – it just looks different. I no longer provide mental health treatment. Instead, I focus on disability advocacy. I speak at conferences about my story. I’ve joined boards of directors, committees, and work groups that focus on disability advocacy. I’ve become involved with pageantry, which gives me an opportunity to talk about disability and mental health. With mental health therapy, I was able to grieve my deep losses, redefine my purpose, and effectively manage my alcohol use. I’ve rebuilt a life for myself that focuses on gratitude, joy, creativity, and intentional goals.
Next Steps and Useful Resources
- For more information about the signs and symptoms of Pompe disease , as well an overview of diagnosis and treatment concerns, an in-depth review can be found here.
- Learn more by reading Simply Stated: Updates in Pompe Disease and Other Glycogen Storage Diseases.
- To learn more about MDA’s Mental Health Hub, visit here.
- MDA’s Resource Center provides support, guidance, and resources for patients and families. Contact the MDA Resource Center at 1-833-ASK-MDA1 or ResourceCenter@mdausa.org
- Stay up-to-date on Quest content! Subscribe to Quest Magazine and Newsletter.
Disclaimer: No content on this site should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.




